Sexual health inequalities are unfair and avoidable differences in sexual health across the population, and between different groups within society.
These inequalities arise and impact opportunities for good sexual health in the most affected groups. The effects of poor sexual health are significant, affecting how people think, feel and act towards sex. This can have a long-lasting impact on mental health, physical health and overall wellbeing.
The State of the Nation Report 2020
The Terrence Higgins trust presented the State of the Nation report of 2020 in partnership with the British Association for Sexual Health and HIV (BASHH) [1]. They believed that an investigation into sexual health across England was long overdue.
The report is sobering, it presents some uncomfortable truths exposing stark inequalities in sexual health outcomes across England.
It presents challenges to the Government, the NHS, the sexual health sector and voluntary and community organisations. The report confirms that once again England has some of the poorest sexual health outcomes in Europe.
Most alarmingly, it found that the burden of poor sexual health is not evenly distributed and that marginalised communities continue to be disproportionally impacted by higher rates of sexually transmitted infections.
Some of the key findings of the report include:
- While some progress is being made – with declines in rates of STIs such as genital warts – other STIs are skyrocketing. Syphilis and Gonorrhoea have increased by 165% and 249% respectively in the past decade
- There are firm structural inequalities, including the impact of poverty – with individuals living in poverty experiencing higher rates of STIs
- There is little research looking at the impact of discrimination, including racism, homophobia and transphobia, on the trends seen in STIs
- Research on inequalities is largely absent. This report found little evidence or data looking at men who have sex with men and who don’t identify as gay or bisexual, as well as trans and non-binary, including gender diverse, people, and sex workers
- There is also a lack of evidence on specific ethnic minority communities – with too much data using the unhelpful ‘BAME’ and “other” groupings
Ultimately, the lack of data in these different areas erases the experience of anyone in these groups, and the voices of people affected by poor sexual health will not be heard without a better understanding in these areas
Better Understanding Inequalities
Groups that are underserved and underrepresented in the sexual health data include:
- Men who have sex with men who don’t identify as gay or bisexual
- Men who have sex with men from ethnic minority groups
- Trans, non-binary, and gender diverse people
- Young gay and bisexual women
- Ethnic minorities who are not captured by broadly defined definitions
- Sex workers
The State of the Nation report confirms that men from ethnic minority communities who have sex with men, as well as people living with HIV, are among those disproportionately impacted by higher rates of STIs.
Sexual Health Inequalities: LGBT+ Communities
Trans men and non-binary people assigned female at birth report lower contraception use and higher rates of teenage pregnancy. [2]
Trans and non-binary people report that the provision of good sexual and reproductive health information is poor. It has been noted by these groups that information is predominantly heteronormative and cisnormative [2].
Young bisexual women report higher rates of chlamydia, unplanned pregnancies and unhealthy sexual behaviour [2].
Young LGBT+ young people (aged 16-25) have higher rates of self-reported STIs. Lesbians (14%), bisexual women (11%) when compared to heterosexual women (4%) [2].
There is still not an all-inclusive, national framework in place to support the sexual health of LGBT+ people. There are many services directed towards gay and bisexual men but far less directed towards gay and bisexual women and those identifying as trans.
What is Being Done to Address the Inequalities?
There is very little robust and targeted information available for trans and non-binary people around sexual health.
The Terrence Higgins Trust recently launched web pages on sexual health, safer sex, healthy relationships, sexually transmitted infections and HIV, specifically for non-binary and trans people.
This has proved successful due to the way it has been developed. The trans and non-binary community were approached by the Terrence Higgins Trust to learn what resources the community were crying out for. This allowed the development of online resources to be in line with what was needed, whilst using appropriate language that is coined by the community itself.
An example of an online resource by the Terrence Higgins Trust
The use of PrEP medication
PrEP (pre-exposure prophylaxis) is a medication that is taken by people at risk of HIV to prevent getting HIV during sex or injection drug use.
The graph below shows data sourced by Public Health England [3]. The disproportionate distribution of HIV infections in England can be seen, with men who have sex with men being the most affected group:
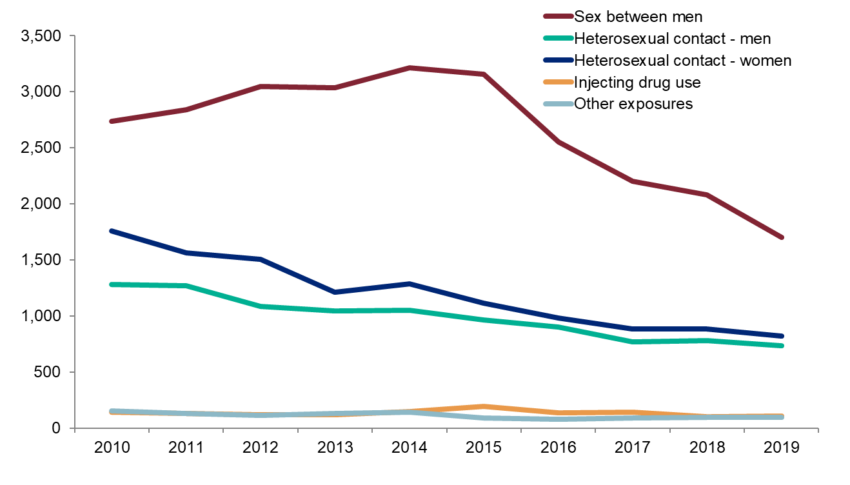
HIV in the UK, infection between 2010 and 2019 (published in November 2020) [3]
However, the rate of infection particularly in the sex between men group has significantly fallen. It is suggested that this may be partly down to an increase in the use of PrEP medication.
Predominantly the people who are accessing PrEP are white, UK born, city-living gay men. This is the group that is most represented in the data presented by Public Health England. Consequently, there are still significant inequalities, despite the drop in HIV cases.
Further inequalities in the access of PrEP medication include [2]:
- 24,255 people were recruited to a PrEP Impact Trial in July 2020. 23,217 (95.7%) of this sample group were gay, bisexual, and other men who have sex with men (MSM). Just 1,038 (4.3%) of the sample were form other groups
- This shows that there is a continuous struggle to effectively engage with non-MSM groups at risk of HIV in PrEP provision
- Additionally, within the MSM group there are inequalities with knowledge access and uptake of PrEP. Men who have sex with men who don’t identify as gay and MSM men from ethnic minority groups are less likely to access PrEP than white and openly gay men
PrEP Campaign for the Black African Community
The Terrence Higgins Trust began an award-winning PrEP campaign which ran from October to November 2020. The campaign was targeted specifically at Black African individuals with the aim of addressing the inequalities in the uptake of PrEP medication.
The campaign was developed through community engagement in the form of surveys to inform what the project should involve.
A website was developed containing PrEP information. The campaign reached over 4 million people online, with 67,800 link clicks achieved through digital adverts that directed people to the campaign webpage.
The PrEP information webpage has been viewed 79,595 times and 1,254 people completed the PrEP self-assessment tool. The self-assessment tool is an interactive resource that asks people about their sexual experience and tells them whether they would benefit from using PrEP or not and if so, offers information on how to access and use it.
Despite high engagement with the campaign, very few Black African people commented directly on posts. The majority sent private messages to learn more about the effectiveness and side effects of PrEP.
Additionally, some users commented to ‘correct’ the campaign believing it was about post-exposure prophylaxis (PEP) and not about PrEP. This demonstrates that although there is a willingness to use the medication, there is an inherent lack of PrEP awareness and knowledge which should not be ignored.
Recommendations
The State of the Nation report makes several recommendations for tackling sexual health inequalities.
Firstly, the sexual health sector should be working with trans organisations and communities to co-produce research and data on the sexual health of trans, non-binary, and gender-diverse people to better understand their experience.
As research is costly, funding must be made available to researchers working alongside affected communities, to fill this evidence gap.
The report recommends that the Government’s new sexual health and reproductive health strategy should have addressing inequalities at its centre. They ask that the new strategy includes actions to understand and tackle the wider socioeconomic determinants that may play a role in driving STI rates in England.
Whilst developing resources to promote accessibility of PrEP, the Terrence Higgins Trust has raised the concern that the medication is only available in sexual health services. This perpetuates inequalities by reducing accessibility. There needs to be a wider range of access points for information and PrEP delivery. It should be available through GPs, community settings and online.
[1] The State of the Nation report. 2020. The Terrence Higgins Trust and the British Association for Sexual Health and HIV
[2] Dr Brady, Michael. 2021. Medical Director, Terrence Higgins Trust and Sexual Health and HIV Consultant, King’s College Hospital and National Advisor for LGBT Health, NHS England
[3] Public Health England, HIV in the UK, infection between 2010 and 2019 (published in November 2020
Register FREE to access 2 more articles
We hope you’ve enjoyed your first article on GE Insights. To access 2 more articles for free, register now to join the Government Events community.
(Use discount code CPWR50)



